Varicose Veins
Superficial veins, appearing blue or purple that have become dilated and twisted.
What Are Varicose Veins?
Varicose veins refer to superficial veins that have become abnormally dilated and twisted. They may appear as blue or dark purple in colour. Although this condition is commonly hereditary, it can also arise without a family history of the condition.
While any vein can become varicosed, the veins most commonly affected are those located in the lower body – particularly the leg veins. This is often due to standing or sitting for extended periods of time wherein the blood is not able to flow properly.
Varicose veins are often the result of one-way valve failure in the major superficial leg veins (saphenous veins). This failure causes vein reflux which prevents the blood from flowing effectively. The pooling of blood in the lower extremities, along with the additional pressure on healthy valves in the veins, leads to the formation of varicose veins.
In many individuals varicose veins only present themselves as spider veins – a mild variation of varicose veins – and is mostly only a cosmetic concern. However, in more severe cases, varicose veins can cause leg pain, discomfort, and may ultimately lead to more serious health issues.
Varicose veins are a common condition affecting 3 in 10 people typically between the ages of 30 and 70 but, with specialised vein removal treatment by a trained sclerotherapist, varicose veins and spider veins can be easily treated.
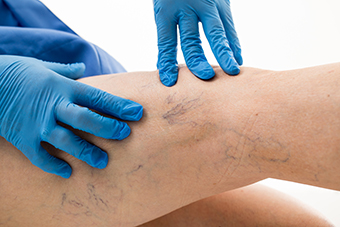

What Are The Symptoms Of Varicose Veins?
The symptoms of varicose veins vary from patient to patient. Some patients are even presented as asymptomatic – meaning that they do no present any symptoms of varicose veins.
However, the most common symptoms of varicose veins include:
- Leg pain and aching
- Swollen feet and ankles
- Itching and eczema
- Tired and aching legs
- Skin darkening around the ankles
- Chronic inflammation
Open sores or bleeding from the varicose veins are symptoms that would warrant an immediate visit with a vein specialist.
What Causes Varicose Veins?
Ultimately, varicose veins are the result of weak or damaged valves in the veins.
Veins are responsible for transporting blood from the body back to the heart to be recirculated. However, to return to the heart, the veins in the lower extremities need to work against gravity. The valves in the veins prevent the blood from flowing backward from the heart.
But if the valves in the veins have become weakened or damaged, the blood will flow backward and pool in the vein. The pooling of the blood, along with the additional pressure on the healthy valves, is what causes varicose veins.
However, varicose veins can also form as a result of past injuries to the legs. Blood clots, pregnancy, and being overweight are also common factors resulting in the formation of varicose veins and spider veins.
How Can Varicose Veins Be Treated?
There are numerous types of treatments to treat and/or remove varicose veins and spider veins.
At Vein Clinic Port Elizabeth we offer the following treatment options:
- The VNUS Procedure
- CLaCS (Cryo-laser and Cryo-Sclerotherapy
- Ambulatory Phlebectomy
- Foam Sclerotherapy
- Micro Sclerotherapy
The above options are available for varicose vein removal and treatment depending on the severity of the condition.
What Are The Complications Resulting From Varicose Veins?
As with any condition there are potential complications that can arise from untreated varicose veins. In the presence of varicose veins or spider veins, the body circulates ‘old’ blood as the blood from the lower body does not travel back to the heart.
By not travelling back to the heart, the pH, carbon dioxide, oxygen, calcium, sodium, magnesium, chlorine and mineral levels in the blood is not converted into a muscle friendly form by the kidneys, liver and lungs.
This imbalance is the primary cause of the leg pain and discomfort in the varicose veins but also increases the risk of further damaging the vein valves, blood clots and ulcers.
Ulcers:
Venous leg ulcers are the most severe varicose vein complication that a patient could experience. As the ‘old’ blood pools in the lower legs, the tissues become deprived of oxygen and nutrition. As a result, skin injuries take longer to heal or do not heal at all and become leg ulcers.
If left untreated, leg ulcers will fail to heal over several years. To successfully heal a leg ulcer the underlying venous reflux needs to be treated.
Venous Eczema:
Patients suffering from venous eczema do not necessarily have to have a history of eczema for the condition to occur. Once again, this condition is a result of the pooling of old blood in the legs.
While steroid creams and skin moisturisers can decrease the chance of venous eczema from occurring, the only long-term cure is to treat the venous reflux.
Superficial Thrombophlebitis:
Blood clotting is a common complication associated with varicose veins. If the varicose veins become hard, red and tender then it is likely that a superficial clot has formed within the vein. It is unlikely that these clots will travel into deeper veins so further complications are unlikely.
However, in severe cases varicose veins can result in a pulmonary embolism. This occurs when a blood clot gets lodged in an artery in the lung preventing blood flow to parts of the lung. This can be fatal if left untreated.
Lipodermatosclerosis
This refers to a non-reversible condition in which the skin around the ankles becomes tough and discoloured. The condition occurs when the scar tissue replaces healthy skin over an extended period of poor nutrition as a result of venous reflux.
While the condition might be irreversible, it does show that the skin is at risk and requires further investigation to plan treatment of the underlying venous reflux condition.
How Can Varicose Veins Be Prevented?
There is currently no treatment to prevent varicose veins or spider veins from forming but there are lifestyle changes that can be made to delay the onset.
These lifestyle changes can also be exercised to reduce the leg pain and other symptoms associated with varicose veins.
These lifestyle changes include:
- Avoid standing or sitting for extended periods of time
- Losing weight if you are overweight
- Walk to exercise your legs daily
- Avoid wearing tight clothing
- Wear compression stockings
- Elevate your legs as often as possible.
- Eat fibrous vegetables and avoid salt.
YOU ARE NOT ALONE
The Vein Clinic Port Elizabeth prides itself in treating the in being the ONLY clinic to offer these procedures in the entire Eastern Cape, including the Garden Route and Umtata.
